Category: Death and Dying
Articles pertaining to death and dying including the dying process and how clinicians determine how much longer a terminally ill patient has to live.
Articles pertaining to death and dying including the dying process and how clinicians determine how much longer a terminally ill patient has to live.

This article provides hospice nurses with practical and evidence-based strategies to discuss end-of-life care with families
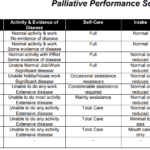
Explore the Palliative Performance Scale (PPS) and its crucial role in end-of-life care. Learn how this tool helps hospice professionals assess patient decline, predict life expectancy, and provide tailored care. Understand the significance of PPS changes in the final six months and how they guide compassionate care decisions.

Losing a loved one to a terminal illness is an incredibly challenging experience. It's a journey filled with emotions, uncertainties, and the need for profound empathy. One crucial aspect of this journey is saying goodbye to your dying loved one and permitting them to pass peacefully. In this article, we'll explore the significance of these acts, which bring comfort to the terminally ill and aid in the grieving process for those left behind. We'll also share three case studies to illustrate the importance of these actions.

Losing a loved one is an incredibly challenging and emotional experience, and witnessing someone's final moments can be overwhelming, especially if you have never been through it before. As a hospice nurse with years of experience, I understand the importance of providing guidance and support during this time. In this article, I want to help prepare you for what to expect during the death visit and explain the role of the hospice registered nurse in the pronouncement process.

As a caregiver or family member, witnessing the final hour of a loved one's life can be a challenging and emotional experience. It's essential to be prepared and understand what to expect. While each person's journey is unique, some common physical changes may occur in the last hour of life. Here's a guide to help you navigate this sensitive time:

Recognizing end-of-life signs can be challenging. This guide outlines key symptoms indicating a terminally ill patient may have less than two weeks, offering crucial insights for caregivers and families.

Losing a loved one is an incredibly challenging experience, and witnessing changes in their behavior and well-being can be distressing. As a hospice nurse, I've supported many families and caregivers through this grim time. One common symptom that may arise towards the end of life is restlessness. In this article, I will explain the different types of restlessness and offer guidance on how to manage them. Understanding these distinctions can provide valuable insights into your loved one's condition and help you navigate the final stages of their life with compassion and care.
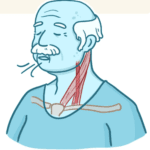
Witnessing a loved one nearing the end of life can be challenging and emotional for a caregiver. One symptom you may encounter during this time is the death rattle. Understanding what the death rattle is, how to recognize it, and how to manage its symptoms can help you provide comfort and support to your loved one in their final days. This guide will explore the death rattle, its significance, and practical tips for managing it.
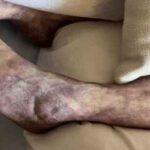
As a caregiver or family member, it can be challenging to witness the changes that occur as a loved one approaches the end of their life. One such change that may occur is mottled skin, also known as livedo reticularis. Understanding what mottled skin is and its significance in the dying process can help you provide the best care and support to your loved one during this time.
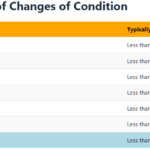
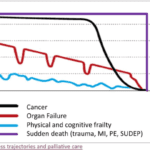
Explore the journey of functional decline in the natural dying process. This article provides insight for caregivers and families, emphasizing the importance of documenting changes to enhance care and decision-making in life’s final chapter.
When a loved one is terminally ill, it can be a perplexing and emotional journey. Understanding the root cause of their declining health becomes paramount. It's a complex puzzle where family members often grapple with questions: Are the symptoms a result of medications prescribed, or are they intrinsic to the terminal disease? This article delves into the critical distinctions between medication side effects and the natural progression of terminal illnesses, offering insights to empower families and caregivers in making informed decisions about their loved one's care.

Discover key indicators for end-of-life care in hospice. This guide highlights ‘trigger words’ that signal a patient’s final days, aiding nurses and caregivers in providing compassionate support during the most critical moments.

I understand how challenging it can be for terminally ill patients to cope with their fear of impending death. It is crucial for both healthcare providers and family members to take these feelings seriously and respond with compassion and understanding. In this article, we will explore the importance of acknowledging a patient's fear of impending doom and discuss actions that families can take to provide peace and comfort during this grim time.

For a non-healthcare professional who has never witnessed death before, it can be unsettling to be present with someone who is nearing the end of their life. However, there are certain signs and observations that you can make using your senses that may indicate that the person you are with may pass away within seconds, minutes, or hours. Understanding these signs can help you provide support and comfort to the individual and their loved ones during this grim time.
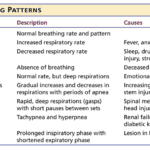

Understanding the final breath: This article explores the critical breathing patterns observed in the last hours of life, offering insights for caregivers and family members to prepare for the end-of-life journey.

Losing a loved one is an incredibly challenging and emotional experience. If you find yourself in the presence of someone in the transitioning phase of the dying process, knowing what signs to look for can be helpful. Although every individual's experience may vary, some common observations may indicate someone is in the transitioning phase. Here's a guide to help you recognize these signs and provide support during this grim time.

Dying doesn’t always hurt. The amount and type of pain there is at the end of life can differ. The specific diagnosis and cause of pain are factors.

Explore the delicate balance of IV fluid use at life’s end. This article discusses the hospice approach, potential risks, and prioritizing comfort over invasive measures. A must-read for families facing tough decisions in palliative care.
Considering tube feeding for a loved one who is in the last year of life. This intervention may not improve quality of life and can lead to discomfort, reduced mobility, and complications. Learn about the risks and make informed decisions for their end-of-life care.

What does a typical day, a typical week look like for a visiting hospice registered nurse case manager look like?

As a hospice registered nurse, I have encountered numerous heartwarming and challenging experiences throughout my career. One of the most memorable encounters was with a dementia patient, Miss Norma Jean Smith, who affectionately called me "Jack." This endearing nickname, born out of her unique perception, became a symbol of the special bond we shared. In the following account, I will share the poignant journey of building trust, providing compassionate care, and embracing the unexpected moments of joy and sorrow in the life of Miss Norma. This story is a testament to the profound impact of person-centered care and the invaluable lessons learned from the patients we are privileged to serve.

One of the hardest portions of the job of a hospice nurse is to identify when a patient has two weeks of life left to live; this can be especially difficult at facilities going through staffing shortages leading to inconsistent caregivers with little to verbally report on a patient’s change of condition. Since being aware of the velocity of declines is extremely important, let’s cover an area that we in hospice (nurses, families, and caregivers alike) can keep an eye on in terms of identifying terminal restlessness which is often a key indicator for one week or less of life.

There is a spiritual connection in hospice, dealing with death and dying forty-plus hours per week. We who are in the field see it often, but there are times when we hear it firmly from the patients and families whom we serve. Let me share the most recent event on Memorial Day, 5/29/2023, week.

I have cared for many terminally ill patients over the years. One question that comes up frequently is should the dying patient be on oxygen at the end of life?
I see it from both sides, from hospice intake personnel as well as the admitting nurse — all had it drilled into them over the years that low oxygen saturation must be treated — to families who see how hospital and nursing home staff rush to put someone on oxygen because of low oxygen saturation.
Contrary to widespread belief, most dying patients do not need oxygen. Here’s why: