Tag: Hospice Nurse
Articles about and for hospice nurses including tips and tricks to provide the best care the terminally ill patient deserves.
Articles about and for hospice nurses including tips and tricks to provide the best care the terminally ill patient deserves.

If you or someone you love has a serious illness that cannot be cured, you may have heard of hospice care. Hospice care is a special kind that focuses on making the patient comfortable and peaceful in their final days. Hospice care also supports the family and caregivers emotionally and spiritually.
When a patient joins hospice care, they will have a special meeting with a hospice nurse. This meeting is called the post-admission visit. It is an especially important visit because it will help the patient and the family get to know the hospice team and learn more about the care they will receive.
This article will explain what to expect and what to ask during the post-admission visit. We will also provide tips and resources to help you and your loved one make the most of this time. We hope this article will help you feel more prepared and confident about the hospice journey.

Discover practical ways to show compassion in hospice care. Learn how small gestures like active listening, gentle touch, and respecting personal space can make a significant difference. Explore the importance of empathy, cultural sensitivity, and self-care for caregivers in providing compassionate end-of-life support.

Discover essential educational topics for hospice nurses during admission and follow-up visits. Learn how to effectively communicate with patients and families, manage symptoms, provide emotional support, and navigate end-of-life care. Enhance your skills to deliver compassionate, comprehensive hospice care.
As a hospice nurse, determining the appropriate frequency of scheduled nurse visits for your patients is essential to providing effective and compassionate end-of-life care. Patients and their families often rely on your expertise to ensure comfort and well-being during this sensitive time. In this article, we'll discuss suggested starting scheduled nurse visit frequencies, when to decrease or increase frequencies, and factors to consider based on patient acuity and changes in their condition.

Navigating hospice eligibility for non-Alzheimer's dementia patients demands a personalized approach. Unlike Alzheimer's, there's no definitive scale, necessitating assessments of functional decline, mobility, communication, incontinence, weight loss, overall condition, and comorbidities. Effective documentation, clinical judgment, and compassionate care are crucial for supporting these patients and families.
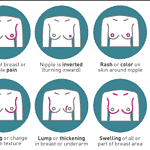
Breast cancer is a tough road, affecting patients and their families deeply. As a hospice nurse case manager specializing in compassionate end-of-life care, I comprehend the significance of offering clear, empathetic guidance to families in this challenging situation. This article delves into the journey through breast cancer, the changes your loved one might undergo, and how to deliver optimal care from diagnosis to life's end.

Navigating the tender journey of hospice care, Compassion Crossing offers guidance on addressing the pivotal question of “when?”—a beacon for caregivers seeking solace and understanding in life’s final chapter.
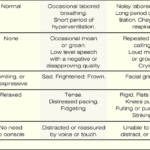
The PAINAD scale is a comprehensive tool that assesses and manages pain in older adults with dementia and delirium. It focuses on observable signs of pain rather than patient self-report, making it particularly useful for individuals who cannot communicate their discomfort
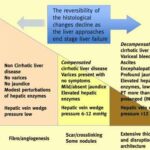
Having a loved one diagnosed with liver disease can be a challenging and emotional journey for both the patient and their family. As an experienced hospice nurse with years of experience in hospice care, I understand the importance of providing compassionate and informative support during this grim time. In this article, we will explore what to expect over the course of liver disease, the changes that may occur in your loved one, and how to provide the best care from onset until the end of life.
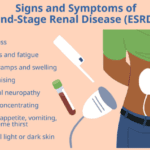
If your loved one has been diagnosed with End Stage Renal Failure, it's natural to feel overwhelmed and unsure about what to expect during the disease. As an experienced hospice nurse with years of experience, I am here to guide you through this journey with compassion and empathy. In this article, we will cover what end-stage renal Failure is, the changes you may observe in your loved one, and how to provide the best care from onset until the end of life.
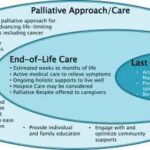
Explore the compassionate approach of hospice nursing assessments, emphasizing patient comfort and dignity over conventional hospital metrics. This article delves into the personalized care that defines hospice evaluations, ensuring a serene transition for patients and families.
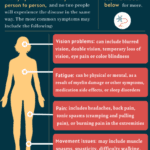
Receiving a diagnosis of Multiple Sclerosis (MS) can be overwhelming for both the patient and their family. As an experienced hospice nurse with years of experience, I am here to provide you with information and support on what to expect over the course of the disease. In this guide, we will discuss the changes your loved one may experience and how you can best care for them from the onset of MS until the end of life.
I know how important it is to provide comfort and support during this challenging journey. One aspect of hospice care that often raises concerns is deprescribing medications. In this article, we'll explore what deprescribing is and why it can benefit patients nearing the end of life.

As an experienced hospice nurse with years of experience, I understand that coping with a loved one's diagnosis of Chronic Obstructive Pulmonary Disease (COPD) can be overwhelming and challenging. In this article, we'll explore what to expect over the course of the disease, the changes you might notice in your loved one, and how to provide the best care and support from the onset until the end.

Losing a loved one is an incredibly challenging experience, and witnessing changes in their behavior and well-being can be distressing. As a hospice nurse, I've supported many families and caregivers through this grim time. One common symptom that may arise towards the end of life is restlessness. In this article, I will explain the different types of restlessness and offer guidance on how to manage them. Understanding these distinctions can provide valuable insights into your loved one's condition and help you navigate the final stages of their life with compassion and care.

As a hospice nurse, I understand the importance of documenting observational signs of discomfort in terminally ill patients. This guide covers recognizing physical and behavioral cues indicating discomfort, even if patients don't express it. It also highlights the benefits of journaling for families and nurses, with tips for effective documentation to enhance patient comfort and care.
Laryngeal cancer is a complex diagnosis for both patients and families. This article aims to provide guidance and support for families new to caring for a loved one with laryngeal cancer. We will discuss what to expect throughout the disease, the changes you may notice in your loved one, and how to provide optimal care from the initial diagnosis to the end.

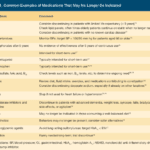
Proper documentation is crucial for hospice nurses to ensure Medicare compliance and maintain the patient's eligibility for services. Auditors, who may not have a healthcare background, review these documents to determine if the patient's condition is terminal. To avoid having the patient removed from service due to improper documentation, hospice nurses should be mindful of the words and phrases they use in their nursing narratives and progress notes. This article will guide what to avoid and why it is essential to paint a picture of a terminally ill patient.

Heart failure is a complex medical condition that can impact the quality of life of patients, especially those in hospice care. As a hospice nurse, assessing the heart failure stage is crucial to providing appropriate care accurately. This article will explore the New York Heart Failure Classification System, its stages, and how to assess patients for their stages. Additionally, we will emphasize the importance of documentation in compliance with Medicare guidelines for terminally ill patients with heart failure.

Medication reconciliation plays a pivotal role in hospice care, ensuring terminally ill patients receive safe medication regimens. This process involves maintaining an accurate medication list to prevent adverse drug events. It's essential at various stages, including admission, recertification, and changes in condition. Healthcare professionals should be familiar with tools like the Beers Criteria and STOPP/START criteria to identify potentially inappropriate medications and prescribing omissions in older adults.

Serotonin syndrome is a potentially life-threatening condition caused by an excess of serotonin in the body. Detecting this condition early is crucial, but it can be particularly challenging when dealing with dementia patients due to communication barriers and the complexity of their symptoms. In this article, we will present three case studies that highlight the early detection and successful management of serotonin syndrome in patients with different types of dementia: Alzheimer's disease, vascular dementia, and Lewy Body Dementia.

Hospice nurses assess the status of the patient's journey towards the end of life every nursing visit. Situations where a reversible condition can drastically impact the patient and the hospice assessment can occur. If it is not caught, it is potentially mistreated, leading to increased discomfort and a faster death, often involving increased suffering. One of the common clues that someone is getting closer to dying is increased agitation and restlessness.
Are you aware of Serotonin Syndrome?

Discover key indicators for end-of-life care in hospice. This guide highlights ‘trigger words’ that signal a patient’s final days, aiding nurses and caregivers in providing compassionate support during the most critical moments.

This article delves into hospice care with Andrew Viozzi, an adept hospice admission registered nurse. Andrew brings valuable insights into the hospice admission process and the broader spectrum of hospice care. Although Andrew's current position revolves around admissions, his extensive experience encompasses case management, preceptorship, mentorship, and the guidance of new hospice nurses. In this article, we dispel misconceptions, highlight the advantages of hospice care, outline the admission procedure, and emphasize the pivotal role of hospice in end-of-life care.