Category: Caregiving Tips
Articles for caregivers of terminally ill patients including how to manage challenging situations.
Articles for caregivers of terminally ill patients including how to manage challenging situations.

Navigating interstate hospice transfers can be complex. This guide explores the process, challenges, and considerations for patients and families. Learn about Medicare regulations, coordination between hospice agencies, and how to ensure continuity of care when moving across state lines during end-of-life care.
Learn how to communicate effectively with healthcare professionals when caring for a loved one with a terminal illness. Improve communication, advocacy, and coping skills to ensure your loved one receives the best care possible.

Managing bowel problems in terminally ill patients is crucial for their comfort and dignity. This guide offers practical tips for caregivers and hospice nurses to address constipation, diarrhea, bowel obstruction, and ascites, ensuring patients' better quality of life.

Dementia is a complex condition affecting millions worldwide. Diagnosing dementia requires the expertise of medical professionals specializing in cognitive disorders. By guiding families and caregivers through the diagnostic process, you can empower them. In this article, we'll explore the steps to find the right specialist for a dementia diagnosis and how families can prepare for the crucial doctor visit.
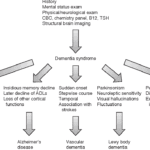
Getting a formal diagnosis of dementia is essential for understanding the condition, accessing appropriate treatments and support services, and ensuring the best possible care. This comprehensive guide explores the importance of a specific diagnosis in predicting patient needs for comfort and quality of life, as different types of dementia require distinct care approaches. Avoid the risks of a generic diagnosis and empower yourself with knowledge.

Caregivers can find it challenging to ensure dementia patients wear their CPAPs overnight. This article offers practical tips and strategies to help caregivers ensure comfortable and uninterrupted CPAP use for their loved ones.

The journey towards the end of life can be a challenging and emotional time, both for the individual facing the end of their life and for their caregivers and family members. One aspect of this journey that may be unfamiliar to many is the presence of self-soothing sounds made by the patient during the transition and actively dying phase. These sounds can be puzzling and sometimes unsettling for caregivers and family members who have never witnessed them. This article will explore self-soothing sounds, why they occur, and how caregivers and family members can distinguish between self-soothing sounds and signs of discomfort.
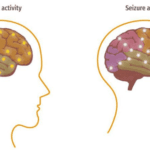
This article delves into the intricate relationship between dementia and seizures, offering insights on identification, safety protocols, and advocacy for caregivers.

This comprehensive guide helps caregivers understand why urinary tract infections (UTIs) are prevalent in dementia patients. It provides practical advice on prevention, early detection, and effective treatment strategies. Empower yourself with the knowledge to provide the best care for your loved ones.

This article is crafted with heartfelt understanding and care, recognizing the challenges you face as caregivers and family members of terminally ill loved ones. Our goal is to empower you with knowledge and practical advice to manage the risk of aspiration pneumonia, a common yet often preventable complication in hospice care.

Deciding on a dementia care facility is crucial. This guide compares personal care homes, assisted living, memory care units, and nursing facilities, detailing Medicaid eligibility, pros and cons, and essential questions to ensure the best care for your family member.

Uncover the importance of regular care plan meetings at healthcare facilities. This guide details participants, goals, benefits, and risks of non-participation.

If you or someone you love has a serious illness that cannot be cured, you may have heard of hospice care. Hospice care is a special kind that focuses on making the patient comfortable and peaceful in their final days. Hospice care also supports the family and caregivers emotionally and spiritually.
When a patient joins hospice care, they will have a special meeting with a hospice nurse. This meeting is called the post-admission visit. It is an especially important visit because it will help the patient and the family get to know the hospice team and learn more about the care they will receive.
This article will explain what to expect and what to ask during the post-admission visit. We will also provide tips and resources to help you and your loved one make the most of this time. We hope this article will help you feel more prepared and confident about the hospice journey.

Facing Creutzfeldt-Jakob Disease (CJD) can be overwhelming, but with the right information and compassionate care, you can navigate this journey with your loved one. This guide is designed to help families new to CJD understand what to expect, recognize changes in their loved one, and provide the best care from onset

Discover practical ways to show compassion in hospice care. Learn how small gestures like active listening, gentle touch, and respecting personal space can make a significant difference. Explore the importance of empathy, cultural sensitivity, and self-care for caregivers in providing compassionate end-of-life support.

Discover how Lion’s Mane, Magnesium Glycinate, Vitamins D3, K2, B1, Folate, C, and MTC Oil can play a role in dementia care. This article delves into the latest research and expert insights on natural supplements that support cognitive function and overall brain health.

Explore the use of ashwagandha and CBD to ease anxiety in dementia patients. Learn about dosages, safety precautions, and real-life stories.

Sundowning, or "late-day confusion," is a challenging experience for individuals with dementia and their caregivers. This phenomenon, occurring in the late afternoon or evening, brings about increased confusion, anxiety, and agitation. Caregivers need to comprehend sundowning and offer compassionate care to ensure the well-being of their loved ones. This article delves into effective pharmacological and non-pharmacological strategies to manage sundowning and create a safe environment.

Navigating the challenges of caring for an elderly parent with dementia can be tough, especially when they resist help. This guide offers practical advice and compassionate strategies to support your loved one while respecting their autonomy and dignity.

Discover the potential side effects of dementia medications and how to support your loved one.

Maintaining routines and consistency can significantly improve the overall well-being and quality of life of a loved one with dementia. As a caregiver, understanding the value of routines and how they can positively impact your loved one's journey through dementia is crucial. In this article, we'll explore why routines matter, how to establish them, and their benefits to patients and caregivers.

Discover gentle methods to encourage dementia patients to bathe. Learn how to create a positive bathing experience, use distraction techniques, and maintain a consistent routine. These compassionate approaches help caregivers navigate hygiene challenges while preserving dignity and reducing stress for both patient and caregiver.

Welcome to our discussion on a topic close to many hearts: the care of our loved ones with dementia. When a family member is diagnosed with dementia, it feels like a part of them slowly fades away. But as they lose parts of themselves, your role in their life becomes even more crucial. This article isn’t just words on a page; it’s a beacon of hope and understanding, shining a light on why your voice, as a family member, is vital in the care of your loved one.

When caring for a loved one with dementia, it's important to approach their needs with empathy and understanding. Dementia is a progressive condition that affects memory, thinking, and communication. As a caregiver or family member, it's crucial to adapt your communication style and strategies to best support your loved one. This article will guide you through the stages of dementia, address common symptoms like anxiety and agitation, provide techniques to reduce caregiver burnout, create a calm environment, and effectively respond to repetitive questions.