Category: Advocacy
Advocacy issues in healthcare especially in the field of hospice
Advocacy issues in healthcare especially in the field of hospice

Discover the essentials of hiring caregivers for terminally ill patients. This guide covers caregiver qualifications, assessing understanding of terminal care, and practical hiring tips.
This comprehensive guide provides valuable insights on how to report and prevent elderly abuse in nursing homes. It serves as a resource for families, guardians, and loved ones to understand their roles and responsibilities in advocating for the elderly. Learn how to empower yourself and ensure the safety and well-being of your loved ones.

Explore how extended hospice care for dementia patients benefits families and saves Medicare money despite regulatory challenges around six-month prognosis rules.

This guide helps families of terminally ill patients comprehend absolute vs. relative risk reduction. It’s a resource for making educated choices about medication continuation, tapering, or cessation in collaboration with healthcare professionals.

This article delves into the challenges faced by family caregivers in hospice and palliative care, offering practical strategies and resources to support them in their indispensable roles.

This comprehensive guide empowers families to navigate care plan meetings for terminally ill loved ones. Learn the significance of these meetings, how to prepare, communicate your loved one's needs, and advocate for their best interests. Gain insights into recognizing when meetings are necessary and the benefits of regular care planning. Equip yourself with the knowledge to ensure your loved one receives personalized, dignified care aligned with their wishes.

When a loved one is facing a serious illness, it can feel like standing at a crossroads. Each path represents a different way to care for them in their time of need. It’s a moment filled with tough choices and deep emotions. This article thoroughly explains hospice care, its philosophy, and the benefits it provides to patients and families facing terminal illness. Learn about the decision-making process, the hospice experience, and how to navigate this difficult choice with dignity and love.

Discover the truth behind the myth that medications can keep terminally ill patients alive indefinitely. This article explores the psychological factors behind this belief and its consequences while providing compassionate strategies to cope with the reality of losing a loved one while ensuring quality end-of-life care.

If you or your loved one has a severe illness, you may have heard about do not resuscitate (DNR) orders. This medical order tells the health care team what to do if the patient’s heart stops beating or they stop breathing. It is an incredibly crucial decision that can affect the quality and length of life. However, there are many myths and misunderstandings about DNR orders that can make it hard to choose what is best for you or your loved one. In this article, we will explain what DNR orders means and why it is important to understand it. We will also debunk the top ten myths about DNR orders and share the facts that can help you make an informed and respectful choice.

You may think that CPR is a miracle that can save anyone’s life, but that is not always the case. CPR is not practical for terminally ill patients, and it can cause more harm than good. In fact, studies show that only about 5% of terminally ill patients who receive CPR survive to leave the hospital. Many of them suffer from brain damage, broken ribs, or infections because of CPR.
This article aims to help you understand the truth about CPR for terminally ill patients. We will debunk ten common myths you may have heard or believed about CPR and provide you with accurate and reliable information. We will also help you make informed and respectful decisions about CPR for your loved one based on their wishes and values.
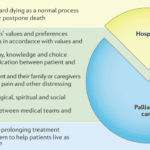
Hospice care is often misunderstood. A common myth suggests that once a patient with a terminal illness enters hospice, they lose control over their care. This article aims to dispel this misconception and highlight the central role of patient and family autonomy in hospice settings. It's important to note that this discussion primarily applies to patients receiving care at home or in non-facility settings, as facility-based patients may have less control over their care decisions.
Discover how to use the CUS tool and Caring Feedback Model to advocate for your loved one's health. This guide empowers caregivers to communicate effectively with healthcare providers, ensuring their concerns are heard and addressed.
Learn how to communicate effectively with healthcare professionals when caring for a loved one with a terminal illness. Improve communication, advocacy, and coping skills to ensure your loved one receives the best care possible.
This article delves into the intricate relationship between dementia and seizures, offering insights on identification, safety protocols, and advocacy for caregivers.

Hospice care in facilities can face challenges due to facility policies, staffing issues, and lack of coordination with hospice providers. This article sheds light on the struggles patients, families, and hospice nurses face in ensuring timely, appropriate care.

Uncover the importance of regular care plan meetings at healthcare facilities. This guide details participants, goals, benefits, and risks of non-participation.

An article that guides families through understanding and exercising their rights to choose the best hospice care for their loved ones, ensuring their final chapter is written with compassion and respect.

Welcome to our discussion on a topic close to many hearts: the care of our loved ones with dementia. When a family member is diagnosed with dementia, it feels like a part of them slowly fades away. But as they lose parts of themselves, your role in their life becomes even more crucial. This article isn’t just words on a page; it’s a beacon of hope and understanding, shining a light on why your voice, as a family member, is vital in the care of your loved one.

Welcome to our guide on hospice care for undocumented immigrants. This article is crafted with the utmost empathy to support family members and caregivers as they navigate the complexities of end-of-life care. Our goal is to provide a clear understanding of hospice services and the unique challenges faced by undocumented immigrants during these tender moments.

When someone you love is extremely sick and needs hospice care, you may feel scared, sad, or angry. You may not know what to do or how to help them. You are not alone. Many people go through this challenging time.
As a hospice nurse, I have met many families who have loved ones in hospice. Some of them are continually active and involved in their care. They ask questions, make decisions, and speak up for their needs. Others are more passive and trusting. They let the doctors, nurses, and staff do whatever they think is best. They don’t say much or ask for anything.
Who do you think gets better care for their loved ones? The active ones or the passive ones?

Caring for a loved one who has a terminal illness can be extremely rewarding but also particularly challenging. You may feel exhausted, overwhelmed, or isolated by the demands of caregiving. You may also feel guilty or anxious about taking a break from your loved one. But you deserve time to rest, recharge, and care for yourself. That is why hospice respite care can be a great option for you and your loved one.
Hospice respite care is a service that allows you to temporarily place your loved one in a facility, such as a hospital, nursing home, or hospice house, where they can receive professional care and support. You can use this time to do whatever you need or want, such as sleeping, working, running errands, visiting friends, or enjoying a hobby. Respite care can last up to five days at a time.

As a family member of a terminally ill loved one receiving care in a facility, you play a vital role in ensuring they receive the best possible care and support during their journey towards a good death. Advocating for your loved one involves understanding their needs, communicating effectively with the facility staff, and staying informed about their care plan. This article aims to guide you on being an effective advocate, asking the right questions, and ensuring your loved one's comfort and well-being.

As an experienced hospice visiting registered nurse, today offered me profound insights from two interconnected perspectives. The first highlights the blind trust we often place in facility nurses and doctors when caring for our loved ones. The second involves the challenges I encountered while advocating for proper end-of-life care for a patient with Alzheimer's.