Managing Dysphagia for Comfort: A Guide for Families
Published on February 7, 2024
Updated on July 6, 2024
Published on February 7, 2024
Updated on July 6, 2024
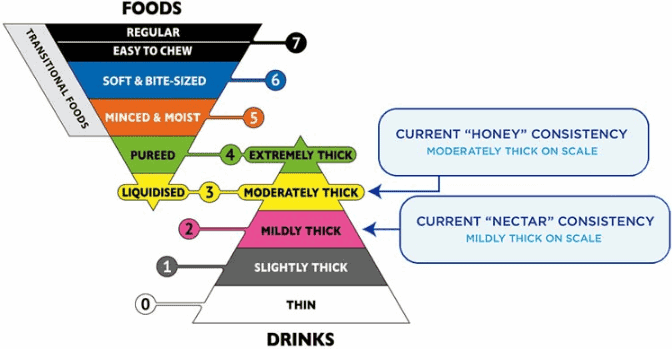
Table of Contents
Caring for a loved one with dysphagia during their end-of-life journey can be challenging, but with the proper knowledge and support, you can provide them with comfort and dignity. Dysphagia, or difficulty swallowing, is a common symptom in terminally ill patients and can lead to complications if not managed properly. In this guide, we will provide you with essential information on managing dietary changes and what to expect and offer helpful tips and tricks to ensure your loved one’s comfort.
If you have a family member who has dysphagia, you might be wondering what it means and how it affects them. Dysphagia is a word that means having trouble swallowing. Sometimes, people with dysphagia feel like food or drinks get stuck in their throat or chest. Other times, they might cough, choke, or drool when they try to eat or drink. This can make them feel scared, sad, or angry.
Dysphagia can happen for several reasons. Sometimes, the muscles or nerves that help us swallow are not working well. This can happen if someone has a disease that affects the brain or the nerves, like a stroke, Parkinson’s disease, or Alzheimer’s disease. Other times, something is blocking the throat or the tube that connects the throat to the stomach, called the esophagus. This can happen if someone has a tumor, a goiter, or a bone spur in their neck.
Dysphagia can make it hard for your loved one to get enough food and water to stay healthy. They might lose weight, get dehydrated, or have low energy. Dysphagia can also make it hard for your loved one to enjoy eating with others. They might feel embarrassed, lonely, or isolated. Dysphagia can also be dangerous because it can cause food or liquids to go into the lungs instead of the stomach. This is called aspiration, and it can lead to infections, breathing problems, or even death.
That is why it is crucial to manage dysphagia and help your loved one feel comfortable and safe. You can do many things to help, such as changing the texture of food and drinks, using special techniques or exercises to improve swallowing, and following the advice of doctors and therapists. In this article, we will give you some tips and information on how to do that.
If your loved one has dysphagia, you might be worried about how they will eat and drink in their final days. You want them to be comfortable and happy, but you also don’t want them to choke or get sick from swallowing the wrong way. That’s why hospice care is here to help.
Hospice care is a special kind of care that focuses on making people feel as good as possible when they have a severe illness that cannot be cured. Hospice care is not only for the person who is sick but also for their family and friends who love them.
When your loved one is in hospice care, they will have a team of experts who will take care of their needs, including their swallowing problems. The team will include a hospice nurse, who will visit your home regularly and check on your loved one’s health and comfort. The nurse will also teach you how to care for your loved one and answer any questions.
One of the things the hospice team will do is to test your loved one’s swallowing ability. They will ask them to swallow various foods and liquids and see how they do. They will also look for any signs of trouble, such as coughing, choking, drooling, or feeling like something is stuck in their throat.
Based on the test results, the hospice team will give you some tips on how to make eating and drinking easier and safer for your loved one. They will also work with you to find out what foods and drinks your loved one likes and dislikes and what makes them feel good or bad.
Here are some changes that the hospice team might suggest for your loved one’s diet:
Soft Foods: Some foods are hard to chew and swallow, especially if your loved one has weak teeth or gums. Soft foods are easier to eat and less likely to cause choking. Soft foods include mashed potatoes, yogurt, scrambled eggs, oatmeal, pudding, and well-cooked vegetables. You can also cut or mash other foods to make them softer, such as bread, meat, cheese, or fruit.
Moistened Foods: Sometimes, foods can be too dry and stick to the throat, making it hard to swallow. Adding moisture to foods can help them slide down more smoothly and prevent choking. You can moisten foods by adding sauces, gravies, dressings, butter, milk, or broth. You can dip foods in liquids before eating them, such as dipping bread in soup or crackers in juice.
Pureed Foods: If your loved one has trouble swallowing, they might need to eat pureed foods, blending into a smooth, thick liquid. Pureed foods are easy to swallow and do not require chewing. You can puree food using a blender, food processor, or hand mixer. You can puree almost any food, such as soups, stews, casseroles, meats, vegetables, fruits, or desserts. You can also buy ready-made pureed foods at the grocery store or online.
Thickened Liquids: Sometimes, liquids can be too thin and fast to swallow, causing them to go into the lungs instead of the stomach. This is called aspiration, and it can lead to infections, breathing problems, or even death. Thickening liquids can slow them down and make them easier to control and swallow. You can thicken liquids by adding special powders or gels that you can buy at the pharmacy or online. Natural thickeners like cornstarch, flour, or baby cereal can also be used. The hospice team will tell you how thick the liquids should be for your loved one and how to measure and mix them properly.
Smaller, Frequent Meals: Eating large meals can be tiring and stressful for your loved one, especially if they have trouble swallowing. Smaller, more frequent meals can be more enjoyable and manageable for them. Instead of three big meals daily, you can offer your loved one five or six smaller meals or snacks throughout the day. You can also let them eat whenever they feel hungry or thirsty and not force them to eat at certain times. You can also make the meals more appealing by using colorful plates, cups, and utensils and adding variety and flavor to the foods and drinks.
These are some of the ways that hospice care can help you and your loved one manage dysphagia and make eating and drinking more comfortable and safer. Remember, you are not alone in this journey. The hospice team is always there to support you and answer your questions. They want to ensure that your loved one has the best quality of life possible and that you have peace of mind.
If your loved one has dysphagia, you know how hard it can be for them to eat and drink. Sometimes, they might cough, choke, or feel something is stuck in their throat. This can make them scared or unhappy. You want to help them enjoy their meals and stay healthy.
Luckily, some products can make eating and drinking easier and safer for your loved one. These products can change how food and drinks look or feel so they can go down more smoothly. They can also help your loved one hold and use their utensils better. Here are some examples of helpful products for dysphagia:
Adaptive Utensils: These are spoons and forks made especially for people with trouble using regular ones. They might have bigger handles that are easier to grip or bent handles that are easier to reach. Some even have sensors that tell when food is too hot or cold. Adaptive utensils can help your loved one feed themselves more comfortably and independently.
Dysphagia Cups: These cups are made especially for people who have trouble drinking from regular ones. They might have lids with small holes or spouts that control the flow of liquid or handles that are easier to hold. Some of them even have straws that can suck up thickened drinks. Dysphagia cups can help your loved one drink liquids more safely and avoid choking.
Thickening Agents: These powders or gels can be added to liquids to make them thicker. Thicker liquids are easier to swallow and less likely to enter the lungs. You can buy thickening agents at the pharmacy or online and follow their instructions. You can also ask your doctor or therapist what thickness is best for your loved one. Thickening agents can help your loved one drink liquids more comfortably and prevent infections.
If your loved one has dysphagia, you might be looking for some ways to make their eating and drinking easier and more comfortable. Here are some tips and tricks to help you and your loved one manage dysphagia and enjoy your meals together.
Dysphagia is a condition that makes it hard for people to swallow food and drinks. It can affect people who have a severe illness that cannot be cured, such as cancer, stroke, or dementia. Dysphagia can cause many problems, such as pain, choking, infections, and malnutrition. It can also make people feel sad, angry, or lonely.
If your loved one has dysphagia, hospice care can help you and your loved one manage it and make it more comfortable. Hospice care is a special kind that focuses on making people feel as good as possible near the end of their lives. Hospice care is not only for the person who is sick but also for their family and friends who love them.
The hospice team will work with you and your loved one to find the best way to deal with dysphagia. They will test your loved one’s swallowing ability, give you tips on changing their diet, and help them eat and drink safely. They will also provide some products to make eating and drinking easier and more enjoyable for your loved one. They will also support you emotionally and answer any questions you might have.
Dysphagia can be hard to cope with, but you are not alone. The hospice team is always there to help you and your loved one. They want to ensure that your loved one has the best quality of life possible and that you have peace of mind.
Dietary Changes through the End of Life Journey
Preventing Aspiration in Older Adults with Dysphagia
The Importance of Caregiver Journaling
Reporting Changes in Condition to Hospice
CaringInfo – Caregiver support and much more!
Surviving Caregiving with Dignity, Love, and Kindness
Caregivers.com | Simplifying the Search for In-Home Care
As an Amazon Associate, I earn from qualifying purchases. The amount generated from these “qualifying purchases” helps to maintain this site.
Take Back Your Life: A Caregiver’s Guide to Finding Freedom in the Midst of Overwhelm
The Conscious Caregiver: A Mindful Approach to Caring for Your Loved One Without Losing Yourself
Everything Happens for a Reason: And Other Lies I’ve Loved
Final Gifts: Understanding the Special Awareness, Needs, and Communications of the Dying