Tag: Nursing Assessment
Articles about the nursing assessment often dealing with a terminally ill patient and the goals of maintaining comfort at the end-of-life.
Articles about the nursing assessment often dealing with a terminally ill patient and the goals of maintaining comfort at the end-of-life.

Learn about the essential elements of a comprehensive hospice admission note. This guide helps registered nurses document crucial patient information, from diagnoses to physical assessments, ensuring the delivery of quality end-of-life care and proper eligibility documentation.

Explore how extended hospice care for dementia patients benefits families and saves Medicare money despite regulatory challenges around six-month prognosis rules.

Discover Bullosis Diabeticorum, a rare skin condition in people with diabetes causing painless blisters. Learn how to identify, treat, and care for loved ones with BD and a terminal illness.
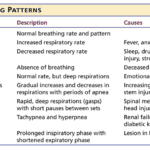

Understanding breathing patterns in end-of-life care is crucial for providing comfort to your loved one. Learn about regular vs. irregular breathing rhythms and when to contact hospice for additional support.
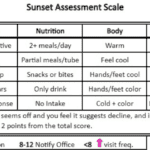
Discover how the Sunset Assessment Scale guides hospice nurses in determining visit frequencies, ensuring compassionate, patient-centered care during the final journey.

Emergency admissions in hospice provide rapid care for patients nearing the end of life. This process involves quick referrals, expedited assessments, and immediate provision of necessary equipment and medications. Hospice teams work efficiently to ensure patients receive comfort and support during this critical time.
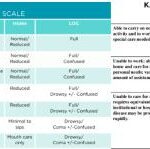

Explore the crucial roles of Karnofsky Performance Status (KPS) and Palliative Performance Score (PPS) in palliative and hospice care. This comprehensive guide helps nurses and caregivers understand these assessment tools, their applications, and critical differences, empowering them to provide more effective, patient-centered care.
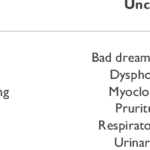

Learn about uncommon opioid side effects like myoclonus and hyperalgesia, and how they impact you and your family. This guide explains these conditions, offers tips for managing them, and highlights the role of hospice in providing comfort and support.

Hospice nurses are crucial in comforting and supporting patients nearing death and their families. This article explores what to expect from hospice care, focusing on patient assessments, educational discussions, and addressing common family concerns.
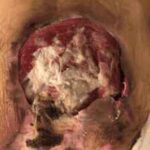
End-of-life wound care is crucial for patient comfort and dignity. This guide covers practical tips for preventing infection, managing symptoms, and supporting caregivers during this sensitive time. Learn how to make wound care a compassionate part of hospice and palliative care.
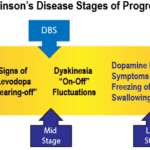
Identifying end-stage Parkinson's for hospice admission can be challenging. This article explores key criteria, including decline in function, weight loss, swallowing difficulties, and mobility issues. Learn how hospice professionals assess patients and utilize guidelines to ensure appropriate and timely hospice care for those with advanced Parkinson's disease.
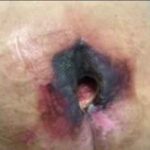
Kennedy ulcers are skin lesions that can develop in individuals nearing the end of life. This guide explores their appearance, causes, diagnosis, and treatment. It offers insights into identifying Kennedy ulcers and providing comfort through pain relief, hygiene, and repositioning. Additionally, it addresses the emotional impact and coping strategies for caregivers and loved ones.

As a hospice admission nurse, asking the right questions is crucial for assessing patients' eligibility and providing compassionate care. This article explores critical questions to understand the patient's condition, decline timeline, hospitalizations, functional abilities, cognitive status, and comorbidities. By gathering this information, nurses can support informed decisions, tailor interventions, and ensure a "good death" for patients and families.
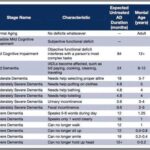
As a nurse who has cared for many terminally ill individuals with Alzheimer's disease over the years, I understand the importance of accurately assessing their functional decline using the Functional Assessment Staging Tool (FAST). The FAST scale provides valuable information about the progression of Alzheimer's disease and helps guide appropriate care planning for patients and their families. In this guide, I will walk you through the process of assessing patients on the FAST scale, starting from stage 1 and discussing when to stop reading the scale for determination. I will also provide three examples of patients at various stages of the FAST scale.
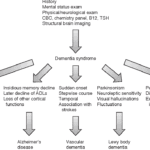
Exploring Hospice Eligibility Criteria for Alzheimer's, Vascular, Lewy Body, Frontotemporal and other Dementias: Empowering Hospice Nurses to Provide Compassionate End-of-Life Care

In the world of healthcare, when a provider writes an order to "Eval and Treat" for hospice, they are asking for a thorough evaluation and a tailored treatment plan. This is specifically meant for patients who are being considered for hospice care. Let's delve into what this means and why it's crucial.
What Does "Eval and Treat" for Hospice Mean?
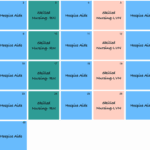
As a hospice nurse, determining the appropriate frequency of scheduled nurse visits for your patients is essential to providing effective and compassionate end-of-life care. Patients and their families often rely on your expertise to ensure comfort and well-being during this sensitive time. In this article, we'll discuss suggested starting scheduled nurse visit frequencies, when to decrease or increase frequencies, and factors to consider based on patient acuity and changes in their condition.

Navigating hospice eligibility for non-Alzheimer's dementia patients demands a personalized approach. Unlike Alzheimer's, there's no definitive scale, necessitating assessments of functional decline, mobility, communication, incontinence, weight loss, overall condition, and comorbidities. Effective documentation, clinical judgment, and compassionate care are crucial for supporting these patients and families.

Navigating the tender journey of hospice care, Compassion Crossing offers guidance on addressing the pivotal question of “when?”—a beacon for caregivers seeking solace and understanding in life’s final chapter.

The purpose of this article is to provide you with some information and guidance about AAAs and how they can be managed in hospice patients.
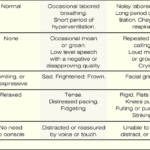
The PAINAD scale is a comprehensive tool that assesses and manages pain in older adults with dementia and delirium. It focuses on observable signs of pain rather than patient self-report, making it particularly useful for individuals who cannot communicate their discomfort
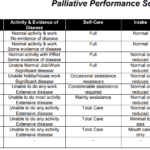
Explore the Palliative Performance Scale (PPS) and its crucial role in end-of-life care. Learn how this tool helps hospice professionals assess patient decline, predict life expectancy, and provide tailored care. Understand the significance of PPS changes in the final six months and how they guide compassionate care decisions.
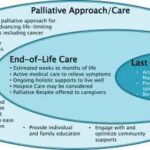
Explore the compassionate approach of hospice nursing assessments, emphasizing patient comfort and dignity over conventional hospital metrics. This article delves into the personalized care that defines hospice evaluations, ensuring a serene transition for patients and families.
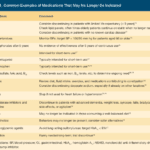
I know how important it is to provide comfort and support during this challenging journey. One aspect of hospice care that often raises concerns is deprescribing medications. In this article, we'll explore what deprescribing is and why it can benefit patients nearing the end of life.