Understanding and Caring for Your Loved One with Prostate Cancer
Published on March 25, 2024
Updated on June 12, 2024
Published on March 25, 2024
Updated on June 12, 2024
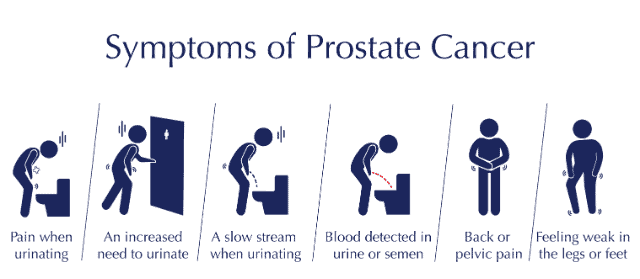
Table of Contents
Navigating the path of prostate cancer can be challenging for both patients and their families. As a hospice registered nurse case manager specializing in end-of-life care, I offer you crucial information, guidance, and unwavering support. In this article, we will delve into the journey of prostate cancer, equipping you with insights about what to anticipate, how to identify changes in your loved one’s condition and the optimal approaches to caregiving from diagnosis to end-of-life. Throughout this article, I aim to present information clearly and empathetically that resonates with your needs and comprehension.
Prostate cancer is a disease that affects some men as they get older. It happens when some cells in a small body part, called the prostate, grow out of control and form a lump. The prostate is a gland that makes a fluid that helps carry sperm. It is located under the bladder, where urine is stored.
Prostate cancer can be complex to notice at first because it usually does not cause any pain or problems. That is why men need to see their doctor regularly and get checked for prostate cancer. The doctor can do a simple test to feel the prostate or take a blood sample to measure a substance called PSA. These tests can help find prostate cancer early when it is easier to treat.
Prostate cancer can grow and spread at different rates. Doctors use stages to describe how far the cancer has gone. Knowing the stage of prostate cancer can help you and your loved one plan for the future and choose the best treatment.
Early Stage: This means that the cancer is still small and only in the prostate. It has not spread to other parts of the body. This stage is also called localized or confined. Men with early-stage prostate cancer may not need treatment right away. They can watch and wait or have active surveillance to see if the cancer changes. If the cancer grows or causes symptoms, they can have surgery or radiation therapy to remove or destroy the cancer.
Localized Stage: This means that the cancer has grown outside the prostate but not very far. It may have reached nearby tissues, such as the seminal vesicles, which are tubes that carry semen. This stage is also called locally advanced or regional. Men with localized stage prostate cancer may need surgery or radiation therapy, along with hormone therapy, to stop the cancer from growing or spreading. Hormone therapy is a type of medicine that lowers the level of testosterone, a male hormone that helps prostate cancer grow.
Advanced Stage: This means that the cancer has spread beyond the prostate and nearby tissues. It may have reached nearby organs, such as the bladder, rectum, or nearby lymph nodes, which are small glands that help fight infections. This stage is also called advanced or metastatic. Men with advanced-stage prostate cancer may need hormone therapy, chemotherapy, immunotherapy, or targeted therapy to slow down the tumor or shrink it. Chemotherapy is a type of medicine that kills cancer cells. Immunotherapy is a medicine that helps the body’s immune system fight cancer. Targeted therapy is a medicine that attacks specific features of cancer cells.
Metastatic Stage: This means that the cancer has spread to distant parts of the body, such as the bones, the lungs, the liver, or the brain. This stage is also called metastatic or distant. Men with metastatic-stage prostate cancer may need the same treatments as those with advanced-stage prostate cancer, along with other therapies to help with pain or other symptoms. For example, they may have radiation therapy or surgery to treat bone pain or drugs to prevent bone fractures.
Prostate cancer can make your loved one feel different from how they used to be. They may have some problems or discomforts that they did not have before. These changes can be complex for you and your loved one to cope with. Here are some of the expected changes that prostate cancer can cause:
Urinary Symptoms: Your loved one may have trouble peeing or need to pee more often or urgently. This is because the prostate is near the bladder, and the cancer can press on it or block it. Your loved one may also leak urine or have blood in their urine. These symptoms can be embarrassing or painful for your loved one. You can help them by being patient and understanding and encouraging them to talk to their doctor about possible treatments or products that can help.
Pain: Your loved one may feel pain in their lower belly, bones, or back. This is because the cancer can grow into nearby tissues or spread to other parts of the body. Pain can make your loved one feel unhappy or angry and affect their daily activities. You can help them by being supportive and comforting and by helping them manage their pain with medicines, heat pads, massages, or other methods that their doctor recommends.
Fatigue: Your loved one may feel tired or weak, even after resting. This is because the cancer can use up its energy or because of the side effects of the treatments. Fatigue can make your loved one feel frustrated or hopeless and prevent them from doing what they enjoy. You can help them by being flexible and respectful and by helping them balance their rest and activity. You can also encourage them to eat well, drink enough water, and exercise moderately if their doctor allows.
Appetite Changes: Your loved one may lose appetite, weight, or taste for certain foods. This is because the cancer can affect their metabolism or because of the side effects of the treatments. Appetite changes can make your loved one feel worried or sad and affect their nutrition and health. You can help them by being gentle and encouraging and by assisting them to eat small, frequent, nutritious meals or snacks. You can also try to make their food more appealing by adding spices, sauces, or flavors they like.
Emotional Changes: Your loved one may feel anxious, depressed, or moody. This is because the cancer can affect their hormones or because of the stress and uncertainty of the situation. Emotional changes can make your loved one feel isolated or misunderstood, affecting their relationships and self-esteem. You can help them by being empathic and attentive and listening to their feelings and concerns. You can also encourage them to seek professional help, such as counseling or therapy if they need it.
Caring for your loved one means being there for them in every way. You want to make them feel better, both in their body and heart and mind. Here are some ways to show your love and support:
Open Communication: Talking to your loved one is crucial. You want to know how they feel, what they fear, and what they want. You also want to share your feelings, fears, and wishes. This way, you can understand each other better and help each other cope. You can talk to your loved one anytime, anywhere, and about anything. You can also write letters, send messages, or make cards for them. The most important thing is to be honest, respectful, and listen carefully.
Pain Management: Pain is one of the most common problems that your loved one may have. Pain can make your loved one feel unhappy or angry and affect their daily activities. You want to help your loved one feel more comfortable and relaxed. You can work closely with the doctors and nurses treating your loved one. They can give your loved one medicines, devices, or other methods to reduce or control their pain. You can also help your loved one by being supportive and comforting and by assisting them to manage their pain with other things, such as heat pads, massages, music, or meditation.
Quality of Life means how well your loved one is living and enjoying their life. You want to help your loved one have the best quality of life possible, even with prostate cancer. You can do this by focusing on what your loved one likes and values and creating special moments together. You can help your loved one do the activities they enjoy, such as reading, gardening, playing games, or watching movies. You can also help your loved one try new things, such as learning a new skill, visiting a new place, or meeting new people. The most important thing is to make your loved one feel happy and fulfilled and to cherish every moment.
There may come a time when the cancer treatment is no longer working, and your loved one is nearing the end of life. This can be an exceedingly difficult and emotional time for both of you. You may feel sad, angry, scared, or numb. You may also have many questions and concerns about what will happen and how to help your loved one. This section will give tips on providing end-of-life care and ensuring comfort and peace for your loved one.
Hospice Care: Hospice care focuses on making your loved one as comfortable as possible in the last months, weeks, or days of life. Hospice care does not try to cure cancer or prolong life but rather to relieve pain and other symptoms, such as nausea, shortness of breath, or anxiety. Hospice care also provides emotional and spiritual support for your loved one and family. Hospice care can be given at home, in a hospital, or at a hospice facility, depending on your loved one’s needs and preferences. You can help your loved one by:
Emotional Well-being: The end of life can be a time of mixed emotions for your loved one and family. Your loved one may feel grateful, peaceful, or relieved but also sad, angry, or scared. They may also have regrets, unfinished business, or unfulfilled dreams. You can help your loved one by:
Prostate cancer can make your loved one’s life overly complicated. They may have many questions, worries, and feelings. They may need a lot of help and support. You may also have your questions, worries, and feelings. You may need help and support too. That is why I am here for you. I am a nurse who has a lot of experience in taking care of people with prostate cancer. I can give you clear and straightforward information about prostate cancer and how to deal with it. I aim to make you and your loved one feel stronger, happier, and more hopeful. Together, we can face the challenges of prostate cancer and find the best way to care for your loved one at the end of their life.
Caring for a Loved One with Terminal Cancer: A Guide for Families
Understanding Cancer Metastasis: A Guide for Patients and Families
American Cancer Society: Prostate Cancer
Prostate Cancer Symptoms, Diagnosis and Treatment
Top 30 FAQs About Hospice: Everything You Need to Know
Understanding Hospice Care: Is it Too Early to Start Hospice?
What’s the process of getting your loved one on hospice service?
Picking a hospice agency to provide hospice services
National Hospice Locator and Medicare Hospice Compare
The Importance of Caregiver Journaling
Reporting Changes in Condition to Hospice
As an Amazon Associate, I earn from qualifying purchases. The amount generated from these “qualifying purchases” helps to maintain this site.
Cancer Caregiving A-to-Z: An At-Home Guide for Patients and Families
Things I Wish I’d Known: Cancer Caregivers Speak Out
CaringInfo – Caregiver support and much more!
Surviving Caregiving with Dignity, Love, and Kindness
Caregivers.com | Simplifying the Search for In-Home Care
As an Amazon Associate, I earn from qualifying purchases. The amount generated from these “qualifying purchases” helps to maintain this site.
Take Back Your Life: A Caregiver’s Guide to Finding Freedom in the Midst of Overwhelm
The Conscious Caregiver: A Mindful Approach to Caring for Your Loved One Without Losing Yourself
Everything Happens for a Reason: And Other Lies I’ve Loved
Final Gifts: Understanding the Special Awareness, Needs, and Communications of the Dying
Providing Comfort During the Last Days of Life with Barbara Karnes RN (YouTube Video)
Preparing the patient, family, and caregivers for a “Good Death.”
Velocity of Changes in Condition as an Indicator of Approaching Death (often helpful to answer how soon? or when?)
The Dying Process and the End of Life
As an Amazon Associate, I earn from qualifying purchases. The amount generated from these “qualifying purchases” helps to maintain this site.
Gone from My Sight: The Dying Experience
The Eleventh Hour: A Caring Guideline for the Hours to Minutes Before Death